Stories of environmental damage and their consequences always seem to take place far away and in another country, usually a tropical one with lush rainforests and poison dart frogs.
In fact, similar stories starring familiar animals are unfolding all the time in our own backyards — including gripping tales of diseases jumping from animal hosts to people when ecosystems are disrupted.
This time we’re not talking hemorrhagic fever and the rainforest. We’re talking tick-borne diseases and the Missouri Ozarks.
And the crucial environmental disruption is not the construction of roads in the rainforest. It is the explosion of white-tailed deer populations.
An interdisciplinary team at Washington University in St. Louis has been keeping a wary eye on emerging tick-borne diseases in Missouri for the past 20 years. Team members include ecologists Brian F. Allan and Jonathan M. Chase, molecular biologists Robert E. Thach and Lisa S. Goessling, and physician Gregory A. Storch.
The team recently developed a sophisticated DNA assay, described in the March 2010 issue of Emerging Infectious Diseases, that allows them to identify which animal hosts are transmitting pathogens to ticks.
“This new technology is going to be the key to understanding the transmission of diseases from wildlife to humans by ticks,” Allan says.
Three new tick-borne diseases
Missouri has three common species of ticks. The black-legged tick (Ixodes scapularis) that carries Lyme disease is found there, but is far less common than in other regions of the country.
Missouri also has American dog ticks (Dermacentor variabilis), which carry Rocky Mountain Spotted Fever, but again this is a less frequently encountered species.
The most common tick is Amblyomma americanum, called the lone star tick because the adult female has a white splotch on her back. It is a woodland species originally found in the southeastern United States whose range now extends northward as far as Maine.
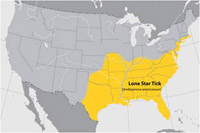
Until recently, this tick, which is an aggressive and indiscriminate biter, was considered a nuisance species, not one that played a role in human disease.
Then, in 1986, a physician noticed bacterial clusters called morulae in a blood smear from a critically ill man that looked like those formed by bacteria in the genus Ehrlichia (named for the German microbiologist Paul Ehrlich). At the time, Ehrlichia were thought to cause disease only in animals.
The bacterium was later identified as a new species, Ehrlichia chaffeensis, and the disease was named human ehrlichiosis. In 1993, E. chaffeensis DNA was found in lone star ticks collected from several states.
Ehrlichiosis typically begins with vague symptoms that mimic those of other bacterial illnesses. In a few patients, however, it progresses rapidly to affect the liver and may cause death unless treated with antibiotics.
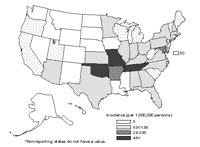
In 1999, a second Ehrlichia species was identified as an agent of human disease. The DNA of the newly identified bacterium was also found in lone star ticks.
Gregory A. Storch, M.D., the Ruth L. Siteman Professor of Pediatrics at Washington University School of Medicine in St. Louis, led the team that identified the second Ehrlichia species. The discovery was described in the New England Journal of Medicine in 1999.
Blood samples from patients in the St. Louis area who might have a tick-borne disease are still sent to Storch’s lab for analysis.
But the ehrlichioses weren’t the only emerging diseases the tick was carrying. In the 1980s, reports had started to trickle in from Missouri, North Carolina and Maryland of an illness accompanied by a bull’s-eye rash. Called STARI, for southern tick-associated rash illness, it resembled Lyme disease but didn’t seem to be as severe.
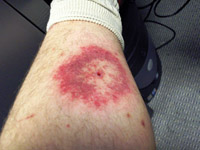
The lone star tick was also incriminated in these cases. STARI is thought to be caused by a bacterium named Borrelia lonestari after its tick vector.
The question
“The question,” says Thach, Ph.D., professor of biology in Arts & Sciences and of biochemistry and molecular biophysics in the School of Medicine, “is where do infectious diseases come from?”
“Most seem to come from nature — they exist in other animals — and then make the leap from animals to people,” Thach says.
Assuming this model applies to the lone star tick diseases, what is their animal reservoir and why are they jumping?
Lone star ticks need blood meals to power their metamorphoses (they go through three stages: larva, nymph and adult) and egg-laying.
They sometimes bite coyotes, foxes and other animals, but their favorite hosts are wild turkey and white-tailed deer.
Especially white-tailed deer, which seem to be playing a major role in maintaining large lone star tick populations and setting the stage for tick diseases to jump to people.
Suspicion grows
Fieldwork conducted by Allan, Ph.D., a postdoctoral research fellow at WUSTL’s Tyson Research Center in the oak-history forests that grace the rolling hills of the Missouri Ozarks, was reinforcing the team’s suspicions about deer.
In forests managed by the Missouri Department of Conservation and by the Nature Conservancy, Allan was looking at the effect on tick numbers of management practices such as selective logging and prescribed burns.

Allan’s results show that management practices sometimes have counterintuitive effects on tick numbers. For example, he reported in the Journal of Medical Entomology in September 2009 that prescribed burns increase tick numbers and human risk of exposure to lone star tick diseases.
But this counterintuitive result makes sense if you follow the deer. A prescribed burn leads to a flush of new plant growth. Deer, which are selective browsers, are attracted by the tender greenery. They flood into the burn sites, and drop blood-sated ticks as they browse.
Getting blood from a tick
Although deer were looking shady, the case against them still was largely circumstantial. Could the scientists get definitive evidence?
Allan found a way. He read about an assay that had been developed in the lab of Jeremy S. Gray, Ph.D., at University College Dublin to identify animal reservoirs of Lyme disease. (“There are twice as many cases of Lyme disease in Western Europe as there are in the United States,” says Thach, “and there is a lot of Lyme research being done there.”)
Allan asked Thach whether his lab would be willing to develop a similar assay for the lone star tick diseases.
“With my colleague Lisa Goessling,” Thach says, “we developed the technique here and used it to analyze the ticks Brian brought in from the woods.”
“The technology for identifying mosquito blood meals has existed for some time,” Allan says, “because they take many blood meals over a short period of time, so the blood is usually still fresh when you capture them. And they keep coming back for another meal, so it’s very easy to capture them.
“It’s much harder to get blood from a tick, which usually takes only one blood meal per life stage,”Allan says. “By the time we capture the tick, eight months to a year may have elapsed. The tick has had a long time to digest that blood, so there may be only a tiny amount of DNA left — if there’s any.”
The team does two assays on the tick DNA: one to identify pathogenic bacteria and the other to identify the animal that provided the blood and with it the bacteria.
Analyzing DNA in the blood
The first step in the assay is to pulverize the ticks to release the DNA, which is then amplified using a procedure called the polymerase chain reaction, or PCR. This provides enough DNA for identification.
Following amplification is a step called reverse line blot hybridization. Probes, which are short sequences of DNA unique to a bacterium or to a host animal, are deposited in lines on a membrane. The membrane is then rotated, and the products of the PCR step — tagged with a chemiluminescent (light-generating) dye — are laid down in lines perpendicular to the probe lines.
Wherever two lines cross, DNA from the tick sample mixes with probes for either bacterial or animal DNA. If the two match, the molecules will bond, or hybridize. When the membrane is later washed, tick-sample DNA that has not hybridized washes off. DNA that has hybridized sticks and shows up as a chemiluminescent spot on the membrane. Reading the spots, tells the scientists which bacteria the tick was carrying and which animal provided its last blood meal.
Assay results showed that most of the nymphal lone star ticks infected with E. chaffeensis fed upon a white-tailed deer in the larval life stage. “So deer are definitely a primary reservoir for this bacterium,” says Thach. “But we also found some kind of squirrel — which we have more recently identified as the common gray squirrel — and what appears to be some kind of rabbit.”
In general, the results suggest deer are probably “weakly competent reservoirs” for the tick diseases, meaning that ticks that bit deer stood only a small chance of picking up one of the pathogens. On the other hand, deer have huge “reservoir potential,” because there are so many of them.
The bottom line: a sprinkling of deer is OK; crowds of deer are a problem.
Too many deer
Are the bacteria that cause the new tick-borne diseases truly new or have they existed for a long time in wildlife reservoirs like the white-tailed deer without causing human disease?
“We don’t know the answer,” Allan says, “but my guess is these tick-borne diseases are probably being unleashed by human-mediated environmental change.”
By human-mediated environmental change, he means deer protection, the human behaviors that have led to an explosion in white-tailed deer populations.

“Some state agencies plant food plots for deer, we’ve created deer forage in the form of crop fields and suburban plantings, and we’ve taken away almost all of their predators — except cars,” Allan says.
To be sure, white-tailed deer were once nearly eliminated from the state. In 1925, there were thought to be only 395, according to the Missouri Department of Conservation. The hunting season was closed that year and again from 1938-1944, and deer were relocated to help re-establish them in the state.
Lonnie Hanson of the Missouri Department of Conservation estimated the herd at 1.4 million in 2009. Nationwide, the pattern is similar. Nobody is sure how many deer there are, but estimates range from 8 million to 30 million, levels everyone agrees are excessive.
“If you had to point to one factor that led to the emergence of tick-borne diseases in the eastern United States, it would have to be these unnaturally large populations of deer,” Allan says.