
The shoulder is the most mobile of our joints but with mobility comes the risk of instability. A system of muscles and tendons must actively hold the humerus against a shallow socket in the scapula. When the arms are overhead this system must work especially hard to stabilize the shoulder and provide power.
Two Washington University in St. Louis scientists are imitating nature as they attempt to solve one of the most difficult problems in orthopedic surgery: reattaching tendon to bone.
Their goal is to improve the success rate of rotator cuff repairs. The rotator cuff is the group of four tendons and muscles that surround the shoulder joint. When it is injured, the tendons tear or detach from the bone.
Commonly thought of as a sports injury — or perhaps the scourge of orchestra conductors — rotator cuff tears actually become more common with age. The highest incidence is in patients older than 60, the scientists say.
For the doctor or surgeon, the big challenge of these injuries is the limited ability of the tendon to repair itself or to reattach to the bone. Reported failure rates for rotator cuff surgeries range from 20 percent to 94 percent.
Younan Xia, PhD, the James M. McKelvey Professor in the School of Engineering & Applied Science, and Stavros Thomopoulos, PhD, associate professor of orthopaedic surgery in the School of Medicine, demonstrated an innovative solution to this problem several years ago, publishing their results in Nano Letters in 2009.
Together with co-principal investigator Leesa M. Galatz, associate professor of orthopaedic surgery in the School of Medicine, the research group has just received more than $2 million from the National Institutes of Health to take the next step toward clinical use of the biomimetic patch.
Over the next few years, they will be testing its success in repairing cuff tears in a small animal model, the rat.
The most flexible of joints
NIH
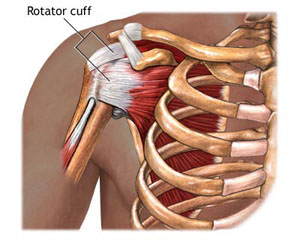
A set of four muscles and their tendons attach to the ball of the humerus, forming what is called the rotator cuff. The cuff becomes susceptible to tears with age. Reattaching the tendon to the bone is difficult because the tendon and bone have very different biomechanical properties and stresses tend to localize along their interface.
Like your hip, your shoulder is a ball and socket joint. But the head of your femur sits deep in its socket in the pelvis, so your hip joint is stable and hard to dislocate.
Not so your shoulder. The ball at the end of the humerus sits in a shallow indentation in the scapula like a golf ball sitting on a tee. This allows your arm to swing much more freely than your leg, but it also means the shoulder joint is inherently unstable.
To solve this problem, the shoulder has an active stability system called the rotator cuff. Four muscles that fan out from the humerus continually pull it back into the socket so that the joint can’t dislocate. Around the ball of the humerus, the tendons form a nearly continuous band like the cuff on a man’s shirt.
The rotator cuff system is in many ways a miracle of biomechanical engineering. The tendons are relatively compliant and stringy, like a rope, and bone is hard and porous, like cement. Some of their mechanical properties differ by a factor of a hundred-fold or more.
“Attaching a compliant material like tendon to a relatively stiff material like bone is a fundamental engineering challenge,” says Thomopoulos.
Merging tendon with bone
Nature has solved this problem by grading the mechanical structure and stiffness of the tissues across the interface between the tendon and the bone.
In an infant, both the bone and the tendon consist of collagen, says Thomopoulos. “Soon after birth, the bone starts to mineralize and a linear gradient forms between the bone and the tendon that slowly stiffens the material and transitions it from hard bone to compliant tendon.”
The difficulty, says Thomopoulos, is that this unique transitional tissue is not recreated after injury.
“If you fall off a ladder and your rotator cuff tears, even if the surgeons goes in and puts the tendon back on the bone, he’s putting the tendon right against bone. You don’t have the graded interface. Biologically, it doesn’t reform.”
As a result, the failure rate for this surgery can be quite high — as high as 94 percent in one study co-authored by Galatz. Many of the patients in the study she published experienced relief from pain, but ultrasound revealed the cuff tear had reopened or a new one had formed.
The biomimetic fix
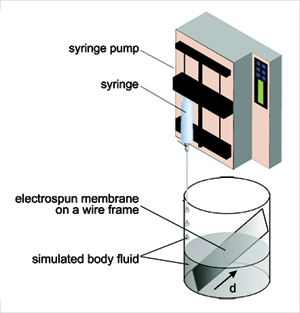
Because the grading between tendon and bone occurs at both microscopic and nanoscopic levels, Thomopoulos teamed up with Xia, an expert in nanotechnology, to find a solution to this problem.
In 2009, Xia and Thomopoulos proposed a simple solution: a temporary scaffold that will guide the healing process along the path it follows during development.
“A few scaffolds have been attempted in rotator cuff repair in humans,” says Thomopoulos, “with only limited success. These patches are fairly compliant materials, even compared to tendon. The hope is that they’ll stimulate a better healing response, but it hasn’t happened yet. Our scaffold approach is to mimic the natural tissue by stepping up gradually in stiffness from tendon to bone.”
The WUSTL scaffold consists of a mat of nanoscopic fibers electrospun in Xia’s lab that mimics the structure of the collagen fibers in a tendon. The mat is then coated with a continuous gradient of hydroxyapatite, a mineral containing calcium and phosphorus that gives strength to bone, so that it is stiff and bone-like toward one end and compliant and tendon-like toward the other.
Finally the scaffold is seeded with adult mesenchymal stem cells, a type of stem cell that can mature into osteoblasts (bone-forming cells) or fibroblasts (cells common in tendon).
The idea is that as the fibers disintegrate over the course of a few months, the mineral gradient will promote the graduated differentiation of the stem cells. Stem cells toward the bone end will be coaxed by the presence of mineral to differentiate into osteoclasts while the stem cells at the tendon end, surrounded by aligned, unmineralized fibers, will form fibroblasts.
“The tendon side is a little bit easier because stem cells tend to go toward the fibroblast-like lineage if you don’t do much to them,” says Thomopoulos.
The presence of either type of cell can be confirmed by looking for markers of each type of mature cell.
Tiny shoulders
“The newly manufactured scaffold looks like a sheet of paper and can be cut to fit the tendon tear,” says Xia.
The team has taken the method as far as they can in vitro and are now ready to try it in a small animal model, the rat.
Galatz, who will perform the surgeries, will create a tear in the rat’s rotator cuff, repair it with a suture, and then lay a piece of the biomimetic scaffold (a few millimeters wide and long) over the repair site.
“You wouldn’t think it,” says Thomopoulos, “but a rat’s shoulder is surprisingly similar to ours. A study done years ago compared the shoulder anatomy of 34 different species, and aside from the primates, the rat bony and muscular anatomy was actually closest to ours.”
“Rats are quadrupeds, but if you observe rats in their cages, they’re reaching overhead quite a bit,” he says.